I can’t pinpoint the exact time that labour began.
At 1.30 am on Tuesday 9th July, I woke needing to go to the toilet (early morning toilet trips had become a regular occurrence in the last few weeks as baby danced around on my bladder). I returned to bed and struggled to get comfortable as I kept experiencing tightening sensations in my pelvis. They weren’t overly intense, but they were noticeable, and I needed to breathe through them. This continued all throughout the early hours of the morning, and while I did my best to rest, I certainly didn’t sleep.
Still, as I was only 36+5 I did not suspect I was in labour, I just thought I was experiencing Braxton Hicks (which I had not yet experienced in my pregnancy), and so when 8.30 am came around, I packed myself up and headed off for work.
At 9.30 am, my shift at work began, and I kept my mobile in my back pocket to continue timing the surges. I shared with some close colleagues how I was feeling, and they reassured me it was likely Braxton Hicks and nothing more. The day continued including me sitting through a meeting and trying to breathe through my surges and time them discreetly with my phone under the table. I ummed and ahhed all morning and early afternoon about whether to ring the hospital but kept telling myself it was a waste of time as they were only Braxton Hicks and nothing more. The hospital would likely just tell me this anyway.
At 4.30 pm, Matt picked me up from work to bring me home. We had to go via the bus interchange to pick up my car and again as I felt a surge rise up I sat in my car and waited for it to pass before driving home.
When we returned home from the walk, I went back to the shower and again stayed in until the hot water ran out. On the shower floor, I noticed some mucous but it wasn’t bloody, and over the last 1-2 weeks I had been losing mucous intermittently so didn’t think too much of it. I returned to the couch, where I suggested we check the hospital bags were in order – ‘just in case’.
At 8.30 pm (13 hours into labour) the surges were still consistently coming every 3-5 minutes and lasting for 40-60 seconds each time. We decided to ring the hospital back and see what they thought. They advised us to come in so they could check me out but were reassuring in that it was likely nothing to worry about. Even so, we put our bags into the car (never expecting to need them) and headed in.

When we arrived, we walked through to the assessment area and paused along the way as I worked through each surge. In the waiting room, I continued this, and it wasn’t long until we were taken through. In the assessment room, a student midwife did my observations, and we were joined in the room by an obstetrics registrar. I explained to her all that had been happening since the morning, and she asked permission to do what she called a visual examination.
As the baby was pre-term, they would not do a vaginal examination.
Instead, they would insert a speculum and visually examine the cervix to see if it had begun to dilate. We consented to the procedure. I utilised my relaxation breathing techniques (and did not find the procedure uncomfortable at all) as the speculum was inserted and the doctor informed us I was 2cm dilated and baby was coming.
The staff left to call our obstetrician and inform him I was in labour and being admitted. They returned shortly after to inform us he had requested that a vaginal examination be performed as this would be more accurate to assess dilation than the visual examination. Again we consented, I utilised my breathing (and again did not find the procedure uncomfortable in the slightest), and we were informed I was, in fact, 4cm dilated.
While a room was organised for me in the delivery suite, we stayed in the assessment room where I continued to breathe through the surges. I even shed a few tears in disbelief that I was actually in labour and our little baby would soon be in our arms.
It was around 10.00 pm (14 ½ hours into labour) that we were taken up to delivery (me in a wheelchair at this stage) and we met our first midwife who would be looking after us. We had requested a room with a bath as we were hoping to have a waterbirth however I was never able to use the bath through the labour or birth as you had to be a minimum of 37 weeks gestation as per the hospital policy.
We explained to the midwife that we were hypnobirthing, and she was very supportive of this and allowed us space. Matt dimmed the room lights and set up our diffuser with lavender oil. We started playing the positive birthing affirmations, which I had listened to daily throughout the pregnancy. I spent hours moving about the room, sitting on a stool and leaning forward on to the bed, sitting on the birthing ball and rolling my hips around, sitting and standing in the shower and even kneeling up over the back of the bed.
Around 2 am on Wednesday morning, Matt was fortunate to enjoy a couple of hours sleep on the fold-out sofa in the delivery room. During this time, the midwife assisted me by using massage and encouraging my relaxation and surge breathing. We were told that the obstetrician would be coming in around 7.30 am to check on us and meanwhile I continued working through the surges.
I spent the early hours of the morning in the shower, finding great relief at spraying the hose on my lower back and also my lower belly. However, as baby needed to be constantly monitored, I was soon limited to spraying my back only as the water on the front of my belly was interfering with the monitoring.
Come morning, we met our second midwife. The obstetrician came in to see us around 8 am and encouraged us that the surges had been measuring very strong. We consented to a vaginal examination (which again I breathed through and did not find uncomfortable).
I was fully effaced; however, still, only 4cm dilated. The same I had been when I was admitted over 12 hours earlier. It was disheartening to hear this as I had now been labouring for just over 24 hours and the surges were much more frequent and much stronger than they had been. He released the membranes and offered us to begin some syntocinon however, we decided we would like to try to continue to labour naturally for a little longer. As baby was happy, he was happy for us to do this and said either himself or a colleague would come by to check on us later in the morning.
I returned to the shower as it was most comfortable for me and the closest to being in the bath as I was going to be able to be. Around 10 am the surges changed, and I began to feel the need to go to the toilet. I moved from the shower to the toilet and was sitting there for not very long when I felt the need to push. Matt got the midwife, and she asked if I would like to return to the bed for another examination. She encouraged me to try and fight the urge to push until she knew how dilated I was.
The examination revealed that whilst the baby’s head was now very low on my cervix (which was fully effaced), I was still only 4cm dilated. This was hard to hear as my surges were so intense, and the feeling to push with each surge could not be ignored. The midwife encouraged me to fight the urges to push, but it was becoming very difficult as I was so tired. I had now been labouring for 26 ½ hours.
Around 11 am one of the obstetrician’s colleagues came in to see how we were going. At this point, I was lying in the bed with Matt on my left sitting on a stool. The obstetrician sat on my right and took my hand. She was very encouraging and even did some visualisations with me, but the surges and sensations were so strong at this point, I was struggling to concentrate. We agreed to begin some syntocinon to help progress. I was now almost 29 hours into my labour, and I chose to request some fentanyl at this point as I felt I was getting no break between the surges and fighting the feeling to push was becoming overwhelming.
I was given the fentanyl at about 11.30, and I recall watching the clock and asking the midwife how long it would take to kick in, I was devastated when she told me 20 minutes. At this point, the surges felt they were rolling in one after the other with no break in between. I was staring down the clock, waiting for 20 minutes to pass and for the fentanyl to kick in.
Sometime around 12.00 pm, our obstetrician returned to have a talk with us. There had still been no progress with dilation, and we needed to discuss our options as I had been labouring for almost 30 hours.
The exhaustion was very overwhelming at this point, and he was concerned that given I had not had any rest for now close to 36 hours. Also, not knowing how much longer until the baby might arrive the chances of either needing an assisted delivery with forceps or an emergency caesarean if the baby became distressed were increasing.
He advised that we consider having an epidural which would allow me some rest and also consent to the syntocinon being increased. We agreed to have a consult with the anaesthetist to be given some more information on the epidural and for the syntocinon to be increased in the meantime.
At 12.30 pm we met with the anaesthetist and anaesthetics registrar to discuss the epidural. We talked about the process as well as the risks and benefits and had the opportunity to ask any questions. We decided not to have one at this point in time but knew they were available if we changed our mind. So with the syntocinon increased, I continue to breathe through the surges. At this point, the sensations were so strong I began to find a different rhythm in breathing through the surges. The breath came in through my nose, and I hummed as loud as I could as I breathed out. I focused all of my energy on the hum as I fought the intense sensations and the increasing urge to push.
At 2.30-3.00pm we met our third midwife. The urge to push was becoming too strong for me to continue to resist, and I was just so exhausted I turned to Matt and requested the epidural. He knew I had never really wanted this and so asked me if I was sure. I know he was afraid of going against my original wishes in case I resented the decision after the labour and birth. I had spent the last 32 hours hypnobirthing and told him I was not feeling pressured into anything. I was simply exhausted yet still determined to have an unassisted vaginal delivery if possible, and I felt having an epidural was the only way I was going to be able to continue to manage the surges given my exhaustion.
We agreed, and within half an hour, the anaesthetics team had returned, the epidural was given, and I was much more comfortable lying on my side.
The positive birthing affirmations continued to play, and I shut my eyes, focused on my breathing and afforded myself a couple of hours of rest. I didn’t sleep in this time but felt incredibly relaxed and content, knowing my baby would hopefully soon be in my arms.
With the epidural in, the midwife began further increasing the syntocinon. Around 5.00 pm, I felt an intense surge of nausea wash over me. I immediately asked the midwife if I was able to have anything for it as I have a massive fear of vomiting (and had been fortunate to not experience any morning sickness during the pregnancy).
She was able to give me some ondansetron, and I felt much better. She then told us she thought I would be ready to push soon and would call the obstetrician down to see us. When he arrived, he talked to us about the progress of the labour (now around 33.5 hours into labour) and explained to us that baby was still happy so we could continue to proceed to aim for a vaginal delivery.
With the epidural now working for around two hours and the syntocinon turned all the way up he was hopeful that I would have made some progress but I was probably still unlikely to be fully dilated. Before examining me, he reiterated that given baby was still happy even if I wasn’t yet fully dilated we would still be able to continue labouring and aiming for a vaginal delivery. Due to the lack of progress up until this point, he was not convinced that I would be fully dilated but was hoping to see some progress.
The OB had barely begun the examination when surprisingly he told us I was fully dilated and baby’s head was right down – I was ready to push.
The midwife began preparing the baby’s bassinet and any other equipment needed for when he was delivered. I felt stunned and emotional knowing it would not be too long before the baby was here (although in the back on my mind reminding myself that pushing is hard work and it could still be a couple of hours before he arrived).
At 5.50 pm, the OB and midwife were ready, and we began with a few ‘practice’ pushes so I could learn a good technique. Through our birth preferences, we really wanted to do mother directed bearing down or pushing; however, due to the epidural, this was obviously not possible. I was so grateful for our amazing midwife who knew how disappointed I had felt that I was not getting the birthing experience I really wanted and had worked so hard to have. Instead of herself telling me when to push she was able to show Matt how to put his hands on belly and feel the surges, so he was able to tell me when they were happening and when I needed to push. They also moved a large mirror to the end of the bed so I could see everything that was happening and the midwife offered to take our camera so Matt could be completely present with me and she captured the birth for us.
I began pushing at 6.00 pm (34 ½ hours into labour). I did three pushes for every surge. Baby’s heart rate began to drop as I was pushing but picked back up between surges so the OB was happy for me to continue and reassured us that should baby need to come out in a hurry he could do that quite easily and there was no going back from a vaginal delivery now. I remember just feeling so determined to push my baby out. With so many other aspects of the birth not going how I wished I was determined that I would push this baby out with no episiotomy and no forceps or assistance.
26 minutes later, at 6.26 pm, Matt left my side to move to the end of the bed. With guidance from the OB, Matt caught our son and placed him on my chest. There are absolutely no words to describe the feelings I had at that moment to be holding my baby safely in my arms.
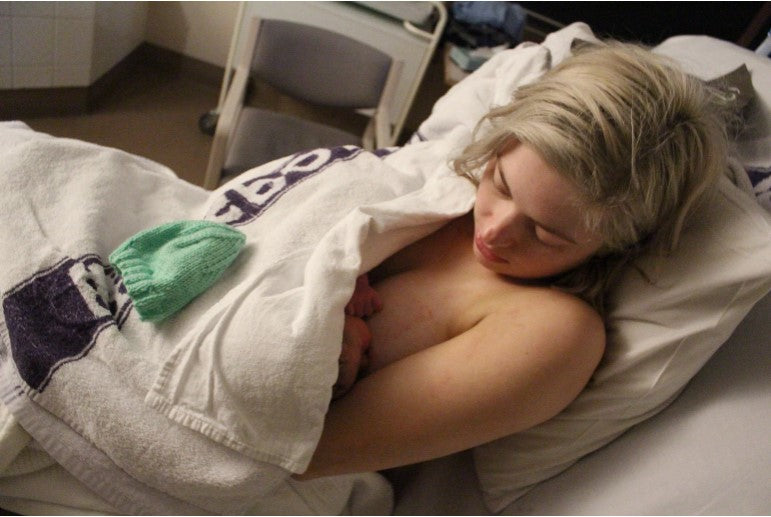
I ended up with a small graze posteriorly, and a tear near my urethra requiring three stitches, however, had a completely easy and pain-free recovery from this.
Quade William was born at 6.26 pm on Wednesday 10th July 2019 (at 36+6 gestation) weighing 3.1kg and measuring 49cm long. Our lives are forever changed for the better. We are so incredibly in love with our perfect little man.









