After three full rounds of IVF and six cycles, Jade and I got the news we had been waiting for; we were going to have our second baby girl due to be born on September 7th 2020.
We knew Jade had to have a caesarean due to the fourth-degree tear she had with our first daughter Billie. The risk of a second, fourth-degree tear was too high, and the complications that come were also significant, so we listened and opted for the c-section.
The pregnancy for the first three months was very routine stock standard morning sickness, tiredness. What was not routine and stock standard was a bloody global pandemic! Covid now meant that Jade had to attend all appointments/scans on her own and I would be sidelined entirely due to all the new pandemic rules.
Month 4/5 came around, and so did the 20-week scan. All seemed good until Jade had her midwife video call later that day. She was told she had some complications: Placenta previa, moderate cord insertion and lastly Vasa Previa.
At the time, the severity of the complications was not explained, and to be honest, we had not heard of most of them, so didn't really know what that meant for our baby. We ended up consulting with a private OB who put some rules in place - Jade could not be further than 15 minutes from the hospital as the risk of a bleed was just too high, and the baby could come out no later than 37 weeks.
August 6th came around, and Melbourne was put into stage 4 restrictions. This now meant that patients in hospital maternity could only have one visitor and only 2 hours per day. August 8th Jade started experiencing cramping and thought she had better get checked out.
It was confirmed pretty quickly that she was in labour and that if the labour continued, they would have to perform an emergency caesarean. I got to the hospital as quickly as possible as I had to wait for someone to look after our 2-year-old.
We were put in a birth suite while the doctors made a decision on what to do as we were only 35 weeks. Thankfully labour stopped on its own, and they were able to administer steroids and make a plan to bring the baby out three days later.
Tuesday, August 11th came around quickly - we were booked for our caesarean and were wheeled down to theatre before lunch. I was put into a holding bay while they prepped Jade and got her blood pressure under control. She mentioned then to the doctors that the baby was moving a lot, but the doctors were having issues finding bub's heartbeat, so they were keen to get me in and baby out.
At 12.35 pm Piper Jade made her dramatic entrance. Breech, septic due to taking a breath and now not breathing. I was removed instantly while they worked on our baby.
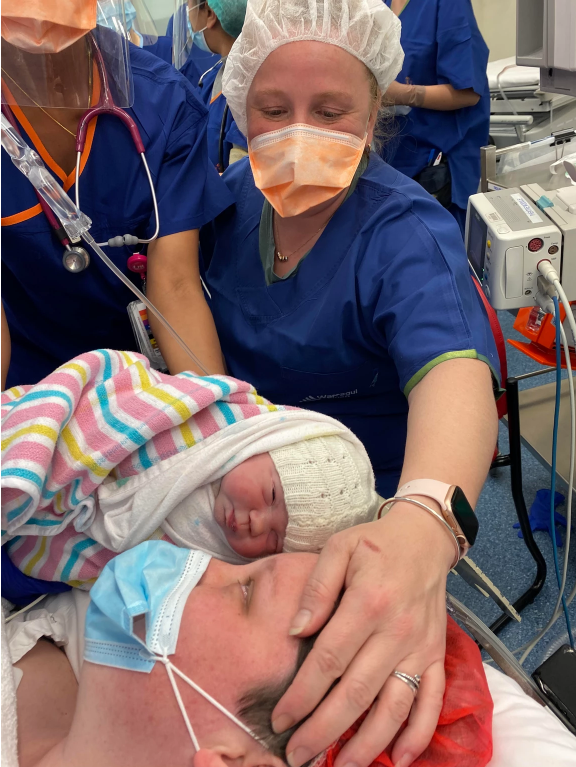

The doctors had Monash ready to send a helicopter for Piper, but finally, after 7 minutes she was able to breathe on her own. We got 1 minute to see her as a family before she was taken to special care for the next 12 days.
Special care Covid rules meant that Jade and I could not be with Piper at the same time. Jade only got to hold piper 20 hours after she was born and I didn't get to hold her for 36 hours. We were not together as a family for 12 more days.

Piper was put on antibiotics right away, fluids, a billi mat for jaundice, and eventually had to have a gastric tube as she could not suck properly. We are incredibly lucky to have our little girl with us now as the odds from the start were against her, but her strength proved time and time again that she was meant to be here.
To all the mums that are experiencing anything like this and feel like you don't have enough information - seek a second opinion you never know. If you feel like something is wrong, speak up and make someone listen. No one listened to Jade when she said she could feel a lot of movement just before Piper was born. That was Piper turning into the breech position, and that was why they could not find her heartbeat. Since they didn't know she was breech, the way she was pulled out resulted in her become septic.








